LSU Health New Orleans Joins AACR Project GENIE
LESLIE CAPO – LSU Health Sciences Center Media Contact Office: 504-568-4806 | lcapo@lsuhsc.edu Image sourced from News and Updates | Project
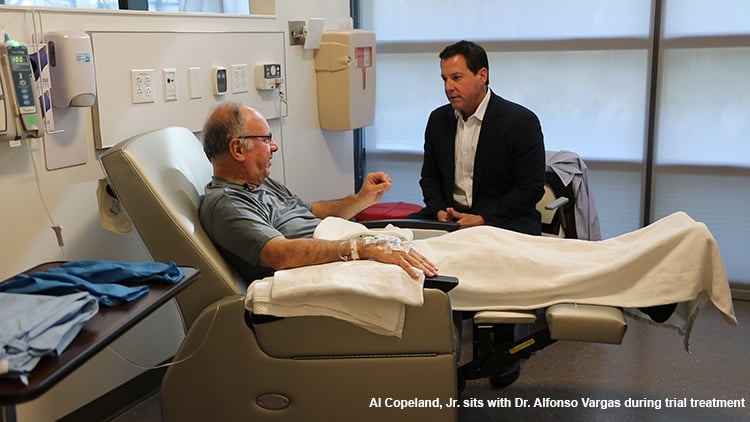

When LSU Health New Orleans enrolled Alfonso Vargas in a clinical trial studying an immunotherapy drug for the treatment of advanced Merkel cell carcinoma, there were no good treatments for this deadly disease. An emeritus professor in LSU Health’s School of Medicine, Dr. Vargas had been diagnosed in the fall of 2016, and as a doctor, he knew his odds for survival were dismal.
“Up to the early 2010s, this lethal variety of neuroendocrine tumors had an average survival rate of 6 to 12 months after diagnosis,” he recalls.
If there is any right time or place to get a cancer like MCC, Vargas’ was it. A confluence of coincidences influenced the course of his cancer.

Vargas was diagnosed at LSU Health New Orleans, where a fellow physician from Colombia, Augusto Ochoa, MD, leads its Stanley S. Scott Cancer Center. LSU Health New Orleans recruited Dr. Ochoa from the National Cancer Institute (NCI), where he had served as Head of the Cancer Immunotherapy Laboratory of the NCI Frederick Cancer Research and Development Center.
The death of legendary New Orleans restaurateur and entrepreneur Al Copeland Sr. from Merkel cell carcinoma in 2008 had resulted in creation of the Al Copeland Foundation, started by his family to carry out their promise to find a cure. They began to raise funds and identify a place doing research worthy of their investment. LSU Health New Orleans Stanley S. Scott Cancer Center was conducting promising research on cancer caused by viruses as well as immunotherapy approaches to treatment. The Center was and remains highly regarded by the National Cancer Institute and a very active site for clinical trials leading to new therapies and treatment advances. The Al Copeland Foundation found its partner.A small, preliminary trial of an immunotherapy drug, which had already been approved for melanoma and certain lung cancers, had shown encouraging results in advanced Merkel cell cancer. The NCI wanted further research with more patients at more sites to see if the treatment results of the drug, pembrolizumab, would hold up as a first-line treatment.

LSU Health New Orleans Stanley S. Scott Cancer Center was selected as 1 of 11 sites to enroll patients in the second trial, and Vargas qualified. His first treatment with pembrolizumab was on November 2, 2016.When a meeting was arranged between Al Copeland Jr. and a patient who was in the trial supported by the foundation, no introductions were needed. Their relationship came full circle as recognition dawned when Copeland saw Vargas. Years before, Dr. Vargas had taken care of one of Copeland’s children, and now Copeland was helping take care of Vargas.
That there were so many connections and so many things had to fall into place so precisely and sequentially, it almost seems that it was meant to be.
Until recently, MCC was treated with chemotherapy, and historically, only 10% of patients with Merkel cell cancer survived 3 years after starting treatment. In contrast, 64% of patients who received pembrolizumab as a first-line therapy during these studies were alive after 3 years.
Vargas is among those with a total response to the drug. “The results have been spectacular. After 18 months of therapy, I was considered tumor-free, not cancer-cured but free of tumors. To be called cured, typically a period of 5 or up to 10 years of being cancer-free has to elapse.”The Food and Drug Administration (FDA) granted approval of pembrolizumab (Keytruda) for advanced Merkel cell carcinoma at the end of 2018. Pembrolizumab, which the the FDA first approved in 2014 to treat melanoma, has now been approved to treat more than a dozen types of cancer, including cancers in a wide range of tissues that have specific genetic features that cause them to accumulate many mutations. For several cancers, including MCC, FDA granted pembrolizumab an accelerated approval, based on promising results from relatively small numbers of patients.

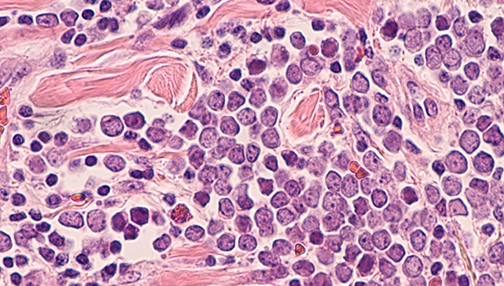
“It’s most exciting to think that our clinicians and patients were able to contribute to approving a drug that effectively treats metastatic Merkel cell cancer, a disease for which there were few if any effective treatments,” notes Augusto Ochoa, MD, Director of LSU Health New Orleans Stanley S. Scott Cancer Center and co-Principal Investigator of the trial.“We are excited that the Copeland-LSU Health New Orleans Partnership in Viruses, Cancer and Immunotherapy was able to be a driving force to bring the first ever Merkel cell carcinoma immunotherapy trial to the Louisiana and Mississippi areas,” said Al Copeland Jr., Chairman of the Board and CEO of Al Copeland Investments.Merkel cell carcinoma (MCC) is an aggressive form of skin cancer. It is linked to exposure to ultraviolet rays, but a high percentage of cases are associated with a virus called Merkel cell polyomavirus. Though rare, the incidence of Merkel cell carcinoma increased by 95% between 2000 and 2013. The five-year overall survival rate has ranged between 14 and 27% for advanced disease. With such poor survival, physician-scientists knew there had to be a better way.
Researchers knew that patients with MCC who had a strong immune response within their tumors tended to have better outcomes and that people who had compromised immune systems were much more likely to develop MCC. They felt boosting patients’ immune responses could help them fight MCC. Certain kinds of cancers are more visible to the immune system, and MCC regardless of its cause, appears to be one of them.

This line of research has really taken off. The approach to managing advanced MCC has changed, with dramatic improvement in survival. Immunotherapies have provided new hope for patients with advanced Merkel cell carcinoma Both avelumab (the first immunotherapy drug approved by the FDA in 2017) and pembrolizumab are immune checkpoint inhibitors. The initial use of checkpoint inhibitors as a first-line therapy has now become the standard or care.It’s much more effective to use immunotherapy and to use it first. MCC will recur in more than 90% of patients who are given chemotherapy, and those who have already received chemotherapy are significantly less likely to respond to subsequent immunotherapy. The researchers have found that the chance of a lasting response is about 10 times higher for immunotherapy, as long as it is given before chemotherapy. As impressive as the results have been, there is more work to be done to further improve outcomes in people with advanced Merkel cell cancer.
“An effective treatment for a devastating disease such as Merkel cell carcinoma using the patient’s own immune system could only be developed through many years of basic and clinical research,” adds Ochoa. “Our participation in this major discovery shows that Louisiana can be at the forefront of research and the discovery of new treatments for cancer.”“What wonderful news it is to all the patients affected with this terrible disease, and to all the men and women who have been working for years to defeat it,” says Vargas. “We also appreciate the ACF as they have been partners in finding a possible ‘cure’ for Merkel cell carcinoma. They are now expanding their philanthropic efforts to cover more patients in the state of Louisiana and to also cover other types of cancers susceptible to treatment with this and other immunotherapies.”
“The Al Copeland Foundation is proud to invest in immunotherapy and this game-changing, lifesaving treatment right here at home,” Copeland says. “While we didn’t win our father’s battle with cancer, we will win the war.”
LESLIE CAPO – LSU Health Sciences Center Media Contact Office: 504-568-4806 | lcapo@lsuhsc.edu Image sourced from News and Updates | Project
https://youtu.be/uN6kyv_QsBMhttps://vimeo.com/807284418?embedded=true&source=video_title&owner=98751849 The success of a Cancer Moonshot doctor and his team in bringing the latest cancer breakthroughs to patients where
LESLIE CAPO – LSU Health Sciences Center Media Contact Office: 504-568-4806 | lcapo@lsuhsc.edu New Orleans, LA – Four LSU Health New
Never miss out on ACF’s latest news or upcoming events!
©2021 Al Copeland Foundation. All rights reserved.